Dear readers, With the launch of e-newsletter CUHK in Focus, CUHKUPDates has retired and this site will no longer be updated. To stay abreast of the University’s latest news, please go to https://focus.cuhk.edu.hk. Thank you.
The Helping Hand of Hydrogels
Bian Liming discovers new forms of hydrogels

Humans are 70% water—but why doesn’t the liquid evaporate or flow away? By studying how the human body, and the natural world, retains that water in a functioning structure, a CUHK biomedical engineer has established promising new implant materials to deliver drugs and heal injuries.
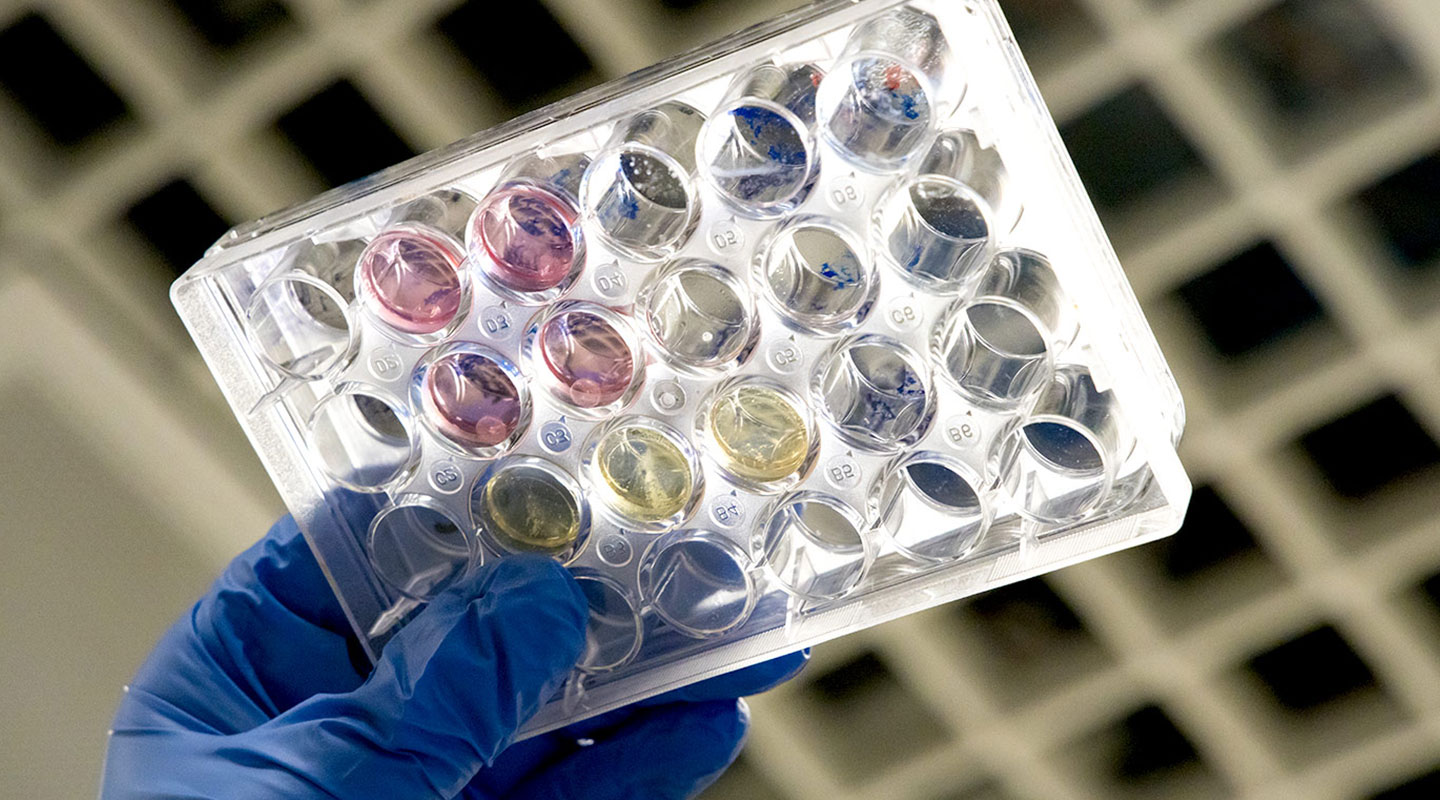
Based on the way human soft tissue functions, Prof. Bian Liming has discovered new properties for hydrogels. Hydrogels are the hydrated polymer networks that form the permeable reservoir to allow nutrients to move into and nourish the cells within; they can act like a liquid to reshape and flow when needed. Hydrogels are solids that function a lot like liquids.
‘A human is like a walking piece of hydrogel,’ Professor Bian says. The chromosomes that contain DNA within our cells, the cells themselves, the organs that contain the cells—all hydrogels.
‘Jelly contains a lot of water, but it won’t flow away. That’s basically what humans are like. if we didn’t have the hydrogels, we would dry out.’
Professor Bian likens his new hydrogels to a ‘smart’ fishing net. Ordinarily the three-dimensional net keeps cells in place. But in the new hydrogel, the connections where the knots of the net connect are dynamic. They are formed from links between molecules that bind and release, allowing the cells to expand the net or even push through it when necessary.
The connections are formed by a guest molecule, adamantane, that inserts into a cup-shaped host molecule, made of a sugar, cyclodextrin. When the guest molecule inserts into the host molecule, it forms a tight bond. But the bond can loosen and be disconnected, then reform again with no damage to the bond after the brief separation.
The raw materials, adamantane and cyclodextrin, can be bought in bulk, and are already used in the pharmaceutical industry to create slow-release drugs. Professor Bian’s team are the first to use those reversible connections to make dynamic hydrogels that can contain cultivable cells.
Cell biologists frequently grow cells in Petri dishes. But those cultures are only two-dimensional, sitting on the surface of the dish. So the way that the cells behave does not replicate the three-dimensional natural environment found in, say, our bodies.
That’s part of the reason why many drugs have been discovered in the lab that kill cancer cells on the 2D level, in a dish. But when they are administered to a real 3D tumor, they do not function as they do in 2D, and fail.
Professor Bian hopes his dynamic ‘fishing net’ hydrogels can be used in the lab to build 3D cancer models that would identify which drugs work in the real world. Since over 90% of drug candidates identified in 2D testing fail, success in this regard would dramatically speed up and reduce the cost of drug discovery.
The hydrogel can also be used to repair injured tissues. There’s potential for stem cells to be cultured within this dynamic hydrogel, then inserted into the cartilage of a damaged knee, to repair it and encourage new cartilage to grow.
Currently, almost all stem cells die within a few hours of being inserted into an injury site, because they have no protection around them to allow them to adapt to their new environment. The hydrogel can afford the stem cells the protection and support they need to survive long enough to prove useful.
‘On the one hand we want to make the structure very dynamic at the microscopic level, and on the other hand we want this material to be very stable at bulk scale,’ Professor Bian notes. ‘That’s a very contradictory environment.’
Professor Bian, who holds a post as an associate professor in the Department of Biomedical Engineering, has also been able to generate hydrogels that are very sticky or take any shape, meaning they can attach to an injury site such as an open wound or a stomach ulcer. The hydrogel can then provide a protective coating at the site of the injury. If the hydrogel is also loaded to contain a therapeutic drug to treat the injury, it could for instance be highly effective in delivering the drug to help an ulcer recover without invasive surgery.
Another common problem with older patients, in their 60s and beyond, is necrotic bone in the femur head. When the hip joint deteriorates through age, the cells in the bone ‘neck’ at the very end of the femur, where the femur inserts into the hip, become dysfunctional. The interior of the femur head and neck therefore becomes necrotic, making it far easier for a patient to break their hip in a fall.
Current treatment involves surgery to remove the dead bone tissue and the liquid that has accumulated. The last resort is a hip replacement, which is highly traumatic and expensive, and has a limited lifespan, meaning the patient may well outlive the replacement.
The new hydrogel can be injected via keyhole surgery into the bone. There, it can fill the holes and cavities that have developed in the bone as it decays, giving it more support. It can also stimulate the growth of new bone. Again, the injection could also contain stem cells to help the bone repair and strengthen. The treatment would at least delay if not obviate the need for a hip replacement.
‘Our injectable material can be delivered without damaging the outer surface of the bone,’ Professor Bian notes. ‘With a tiny puncture, you can deliver the drugs and stem cells into an enclosed anatomical site.’
By infiltrating the bone, the injected hydrogel forms a far more effective treatment. Bone cells, stem cells and immune cells can enter an accommodating environment—speeding up healing.
By Alex Frew McMillan
Photos by Eric Sin
This article was originally published on CUHK Homepage in Oct 2019.