Dear readers, With the launch of e-newsletter CUHK in Focus, CUHKUPDates has retired and this site will no longer be updated. To stay abreast of the University’s latest news, please go to https://focus.cuhk.edu.hk. Thank you.
A Pathfinder in the Hearty Chamber
Huang Yu sheds light on blood vessel dysfunctions

Heart attacks, strokes and kidney failure have a common cause: dysfunction found in the endothelial cells that line the inside of blood vessels. The poor performance of those lining cells sets in motion a cascade of events in the body that ultimately can lead to hardening of the arteries and the formation of blood clots.
It has been the work of Prof. Huang Yu to analyze the chemical pathways that cause those endothelial cells to malfunction. Ultimately he hopes the results can lead to drugs being repurposed to reverse that harmful effect, protecting organs such as the heart and kidneys.
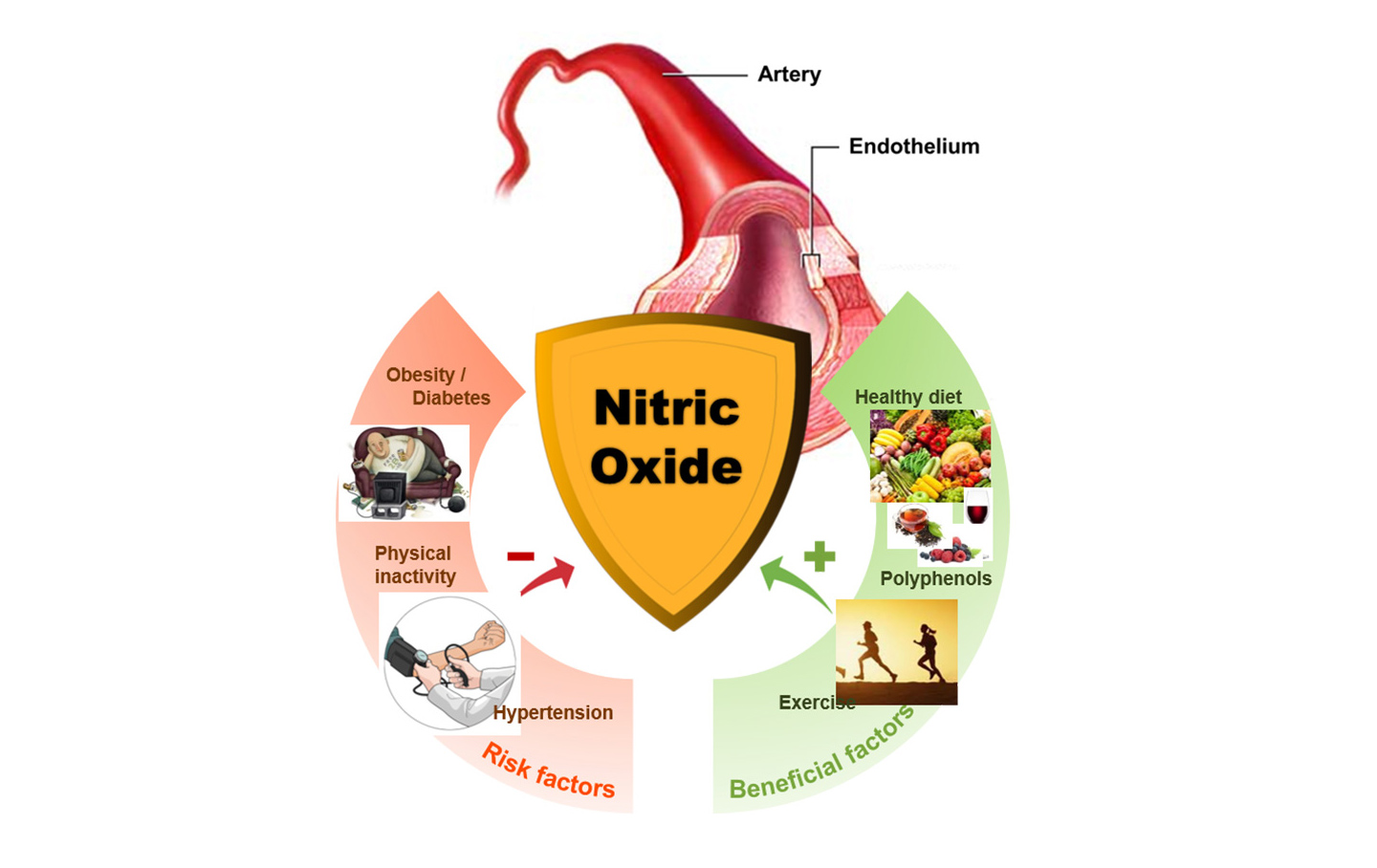
The chemical nitric oxide is key among the stimulants of the endothelial cells, and a focal point of Professor Huang’s work. Nitric oxide is an anti-inflammatory gas molecule, so its production is essential in regulating damage to the cardiovascular system. The endothelial cells, which line not only blood vessels but also the lymphatic system, emit the chemical. It then curbs the contraction, growth, aggregation and inflammation of surrounding smooth-muscle cells, avoiding vascular damage.
But nitric oxide has a very short life, just a couple of seconds long. People with high blood pressure, diabetes, obesity and hardened arteries normally don’t have proper production and function of nitric oxide. Prolonging or stimulating its existence therefore aids a patient’s health.
Scientists have been aware of the role of nitric oxide since the mid-1980s, and particularly since 1998. That’s when three Americans won the Nobel Prize for medicine as a result of their studies showing that nitric oxide acts as a signalling molecule in the cardiovascular system, provoking the relaxation of blood vessels.
Studying how those networks work, and how the production of nitric oxide is reduced or impaired in patients with cardiovascular damage, has been the focus of Professor Huang’s work over the course of the last 15 years. Professor Huang’s main goal is to explain how the network functions when it leads to vascular diseases. That would then suggest how diseases are likely to progress and provide targets for therapeutic intervention.
“Nitric oxide controls the ‘bad guys’ when you’re healthy,” Professor Huang says. ‘Then when, for whatever reason, you produce too many free radicals in your blood vessels, nitric oxide starts to lose its capacity of protecting blood vessels.’
Most recently, he and his postdoctoral fellow Wang Li discovered and proved that the Hippo signaling pathway, which tells endothelial cells how to react, responds differently to varied patterns of blood flow. A straight blood vessel with normal blood flow can stimulate the endothelial cells to produce nitric oxide.
But when blood vessels are curved or arched, or have narrow branches, the flow gets disturbed. This then causes greater production of the free radicals that induce inflammation, as well as reducing the production of beneficial nitric oxide.
The results were recently published in the journal Nature, the most-influential academic journal of its kind. Uncovering how the Hippo pathway signals to other cells will allow for the screening of existing small-molecule drugs to see if they are effective in targeting the pathway in the treatment of atherosclerosis.
The government’s Collaborative Research Fund decided the work was important enough that it granted HK$7.7 million (US$990,000) towards its study, investigating how physical exercise helps with vascular health. It was the first study of the topic ever conducted in Hong Kong. The fund then extended its support to include the investigation of how diabetic animals – as usual, the study chose mice – have impaired nitric oxide production in their endothelial cells.
Exercise, Professor Huang showed, counteracts the effects of the diabetes and causes the endothelial cells to function normally, something he calls ‘remarkable.’ He is now investigating how the ‘cross-talk’ functions between the blood vessels and the body’s organs such as adipose tissue and skeletal muscle. That process, for now, remains largely unknown. The Collaborative Research Fund has recently granted HK$6.8 million (US$880,000) to support this study.
Many pharmaceuticals can help stimulate the production of nitric oxide. For example, Vitamin D is also very effective in preserving nitric oxide and preventing oxidative stress to the vascular wall. Professor Huang also started studying why polyphenols from green or black tea, red wine and several Chinese herbs stimulate the production of nitric oxide, work that the Hong Kong Food and Health Bureau has sponsored.
More recently, Professor Huang’s team have discovered that drugs designed to prevent high blood pressure and also diabetes have the additional effect of preserving the production of nitric oxide in endothelial cells. Professor Huang, who is director of basic sciences at the Institute of Vascular Medicine at CUHK and holds a professorial position in the School of Biomedical Sciences, now oversees 16 other scientists and postgraduate students. Each one is targeting a different way that our blood vessels and metabolic organs function.
Now he is working closely with clinicians to see if that knowledge can be put to use in patients with diabetes, hypertension or atherosclerosis.
‘I like to do clinically relevant basic research,’ Professor Huang says. Ultimately, he hopes, the theory will lead to very profound practice.
By Alex Frew McMillan
This article was originally published on CUHK Homepage in Jun 2017.