Dear readers, With the launch of e-newsletter CUHK in Focus, CUHKUPDates has retired and this site will no longer be updated. To stay abreast of the University’s latest news, please go to https://focus.cuhk.edu.hk. Thank you.
Fighting Liver Cancer from Within
Alfred Cheng’s epigenetic treatment defeats liver cancer’s specialized defences

Liver cancer is a calculating killer. Its tumours have their own defences that prevent a cancer victim's body from defeating the disease. But thanks to the investigative epigenetics of Prof. Alfred Cheng Sze-lok, that may be about to change.
The leading form of liver cancer is hepatocellular carcinoma, the third-largest cause of cancer deaths worldwide. The cancer's prevalence is highest in East Asia, partly as a result of hepatitis B infections, but is increasingly common in Western nations as well due to the rising level of diabetes and obesity.
The existing treatment for that form of liver cancer involves immunotherapy. The drugs contain immune-checkpoint inhibitors, which activate cancer-killing T cells. The cancer suppresses those T cells, so stimulating them can shrink tumours and increase survival rates.
However, only around 15% of patients respond to immunotherapy. One problem is that liver cancer is a 'cold' cancer that walls itself off and prevents T cells from entering the tumour. The cancer also co-opts host cells to suppress T cells.
Professor Cheng has striven to find out how those defences work, and therefore how they can be overcome. His investigation led to the discovery of an epigenetic regulator, an enzyme known as histone deacetylase 8, or HDAC8. To protect the cancer, HDAC8 prevents the production of chemokines, a molecular signal that encourages T cells to come to the body's assistance.
When mice are treated with a drug that inhibits HDAC8, chemokines are expressed in the normal way, and T cells finally start being able to infiltrate the tumour. Professor Cheng likens it to police finally being able to break into Kowloon Walled City, a former citadel within Hong Kong that for decades functioned as a law unto itself.
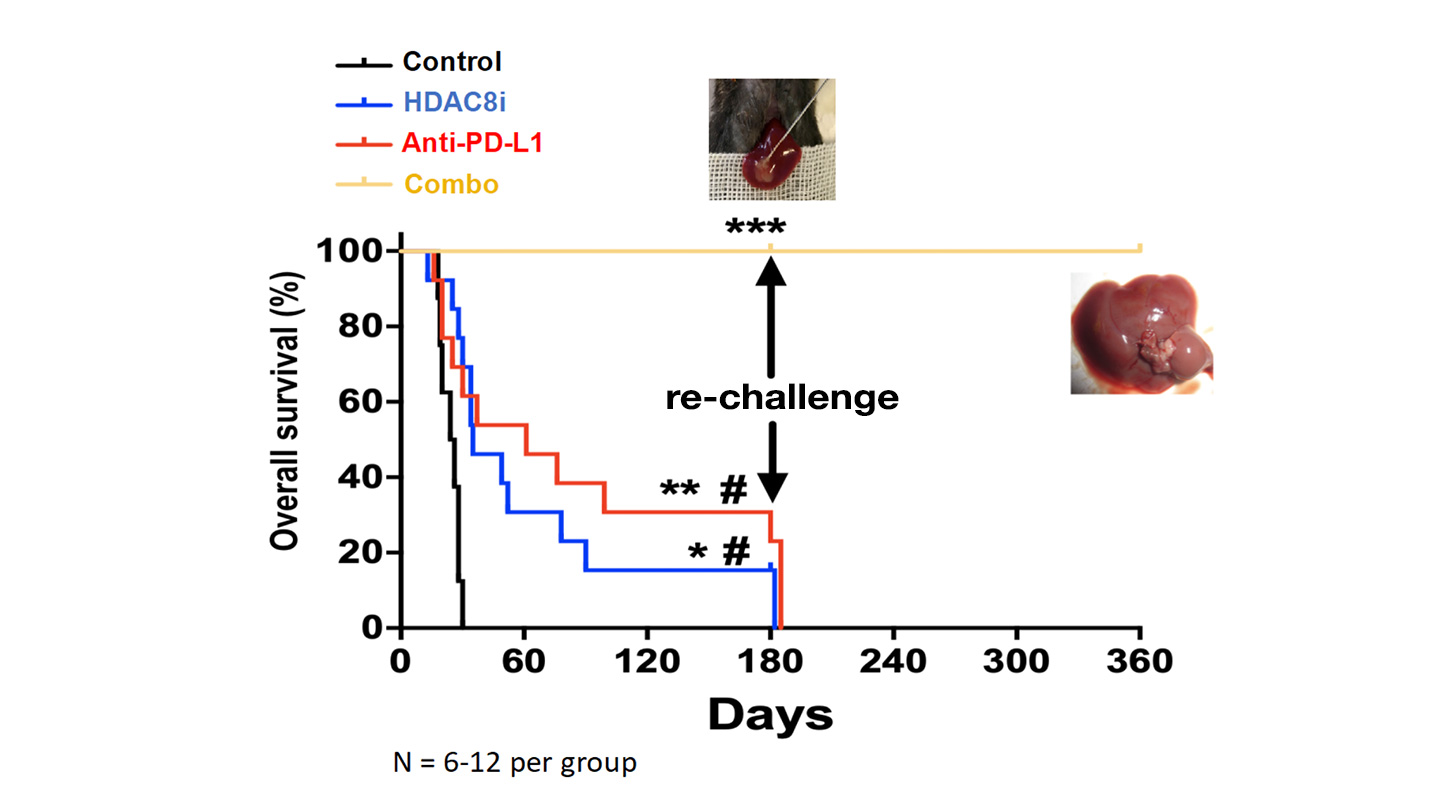
According to lab results shown in the graph above, mice that are implanted with a liver tumour all die within 30 days without treatment. When treated with immunotherapy on its own, the animals survive longer, but all die within 180 days. Likewise, they live longer with epigenetic treatment on its own, but all the animals die within 180 days. When mice are treated with both immunotherapy and epigenetic treatment, all the animals survive longer than 360 days.
'I was quite surprised, but we re-tested it,' Professor Cheng says. 'The duration of the effect is very long.'
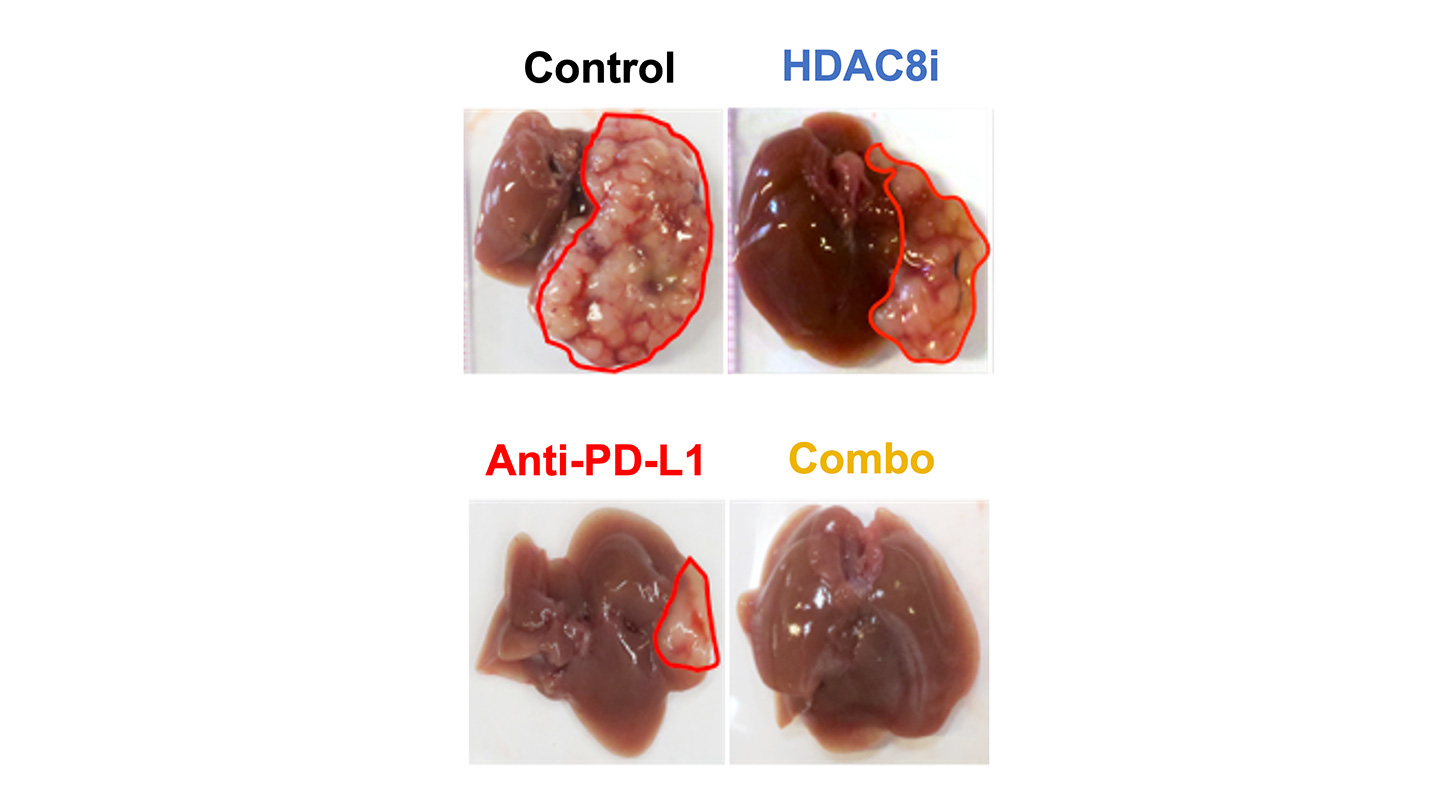
Dissection (pictured above) reveals that when mice are given one form of treatment, the cancer shrinks but remains present on the liver. When mice are given both immunotherapy and epigenetic treatment, the cancer is eradicated, leaving only a perfectly healthy liver, which can recover. The findings were recently published in the journal Science Translational Medicine.
Professor Cheng discovered the importance of HDAC8 by investigating which epigenetic genes are active in two animal models: mice that are genetically bred to become obese and develop liver cancer; and mice that develop liver cancer because they are fed with a high-fat, high-carb diet, the equivalent of Coca-Cola and hamburgers.
The team started out with a list of 115 genes to investigate. The HDAC8 gene was the only one 'upregulated' in both experiments. 'We found that it has indeed very prominent tumour-promoting abilities,' Professor Cheng explains.
The epigenetic work takes the study of cancer beyond what's going on inside the tumour cell to look at the broader immune microenvironment. Unlike our genetics, which are fixed and determine issues such as our eye colour, the field of epigenetics studies genes that are expressed given the influences exerted on them.
'Epigenetics is a totally different ballgame,' Professor Cheng says. Gene expression often 'can be reversed, and the damage is not permanent. That's why I wanted to study epigenetics.'
It's likely that the same treatment would work for other 'cold' or immune-excluded cancers, a category that includes ovarian and pancreatic cancers.
'They also have a high expression of HDAC8 contributing to the coldness of the tumour,' Professor Cheng notes. 'Targeted epigenetic treatment may also be effective.'
The studies in mice have yet to be followed up with human clinical trials. Professor Cheng is collaborating with a drug-development team in Germany, who have produced a series of drugs that can deliver the treatment. Professor Cheng and colleagues from CUHK's School of Pharmacy will now test which of the German-developed drugs is most effective in mice.

The profile of the drug, if it works, will then need to be adapted for human use. Professor Cheng, who is the chief of cancer biology and experimental therapeutics in CUHK's School of Biomedical Sciences, is applying for funding to work on that formulation, which may take around a year.
Professor Cheng estimates that, if all goes well with the safety profile and delivery of the drug, a human trial could begin within three years. If that in turn goes well, work could begin for a drug for clinical use.
Around 70% of liver-cancer patients produce high levels of HDAC8. 'It can be quite beneficial to a substantial portion of patients,' Professor Cheng says.
Such drugs would be part of the progression towards precision medicine, in which patients are treated differently depending on their genetic makeup and disease profile. Every person has their own different tumour. This way, they would not have to fight the disease alone.
By Alex Frew McMillan
Photos by Eric Sin