Dear readers, With the launch of e-newsletter CUHK in Focus, CUHKUPDates has retired and this site will no longer be updated. To stay abreast of the University’s latest news, please go to https://focus.cuhk.edu.hk. Thank you.
Zero Tolerance for Re-bleeding
James Lau’s quest to perfect endoscopic surgery

James Lau Yun-wong, Professor of Surgery at CUHK and Director of the Endoscopy Centre at Prince of Wales Hospital, has been focusing his clinical research in the management of acute upper gastrointestinal (GI) bleeding since the early 90s. Three decades ago, Hong Kong’s rate of incidents of acute GI bleeding topped the world. Both the rates of surgery for patients suffering from bleeding ulcers and that of mortality were high. Over the years, the research done by Professor Lau and his team at the Prince of Wales Hospital has brought endoscopic treatment of peptic ulcer to a new level with a significant reduction in further bleeding (from 20% to less than 4%), the requirement for surgery (from 10% to 1%) and deaths (1%) in patients with upper gastrointestinal bleeding.
Professor Lau published his landmark case on the comparison of endoscopic treatment and surgery in patients with recurrent bleeding from their peptic ulcers in 1999 based on his five-year study under strictly controlled manner. The study showed that endoscopic treatment helped to avoid surgery in 75% of patients with recurrent bleeding. In the following year, another remarkable finding was presented by Professor Lau on the use of proton pump inhibitors (PPI) after endoscopic therapy to reduce the chance of re-bleeding. This involves using a high dose of drug to suppress gastric secretion. Results from several early attempts to show the effectiveness of PPI were inconclusive. Professor Lau noted that in these early studies endoscopic treatment was either not used or used with insufficient patient samples, or the studies lacked discrete outcome variables. The key to Professor Lau’s success lies in his carefully designed clinical trials with randomized, double-blind and placebo-controlled methods to avoid the inadequacies found in the earlier studies.
Both his papers were published in The New England Journal of Medicine and widely cited. His work has brought distinct changes and improvements in medical practices. Endoscopic therapy is now the first-line treatment of upper GI bleeding, and PPI a common practice in reducing re-bleeding after endoscopy.
Over the past few years, Professor Lau has been striving to further reduce the rate of recurrent bleeding among high-risk patients to zero.
High-risk patients refer to those patients with larger-size ulcers and the elderly. They are usually less operable and more susceptible to comorbid diseases. Despite the combined use of PPI and endoscopic therapy, there are still substantial risks of recurrent bleeding. Endoscopic hemostasis, a main type of endoscopic therapy involving the performance of surgery through endoscope with various techniques and tools, is an effective means to control bleeding in ulcers. However, any recurrent bleeding after endoscopic hemostasis to bleeding peptic ulcers would increase the risk of mortality by threefold. A less invasive procedure performed in interventional radiology──Transcatheter arterial embolization (TAE)──has been proposed to be an alternative which involves the using of angiography, catheters and coils to prevent further bleeding.
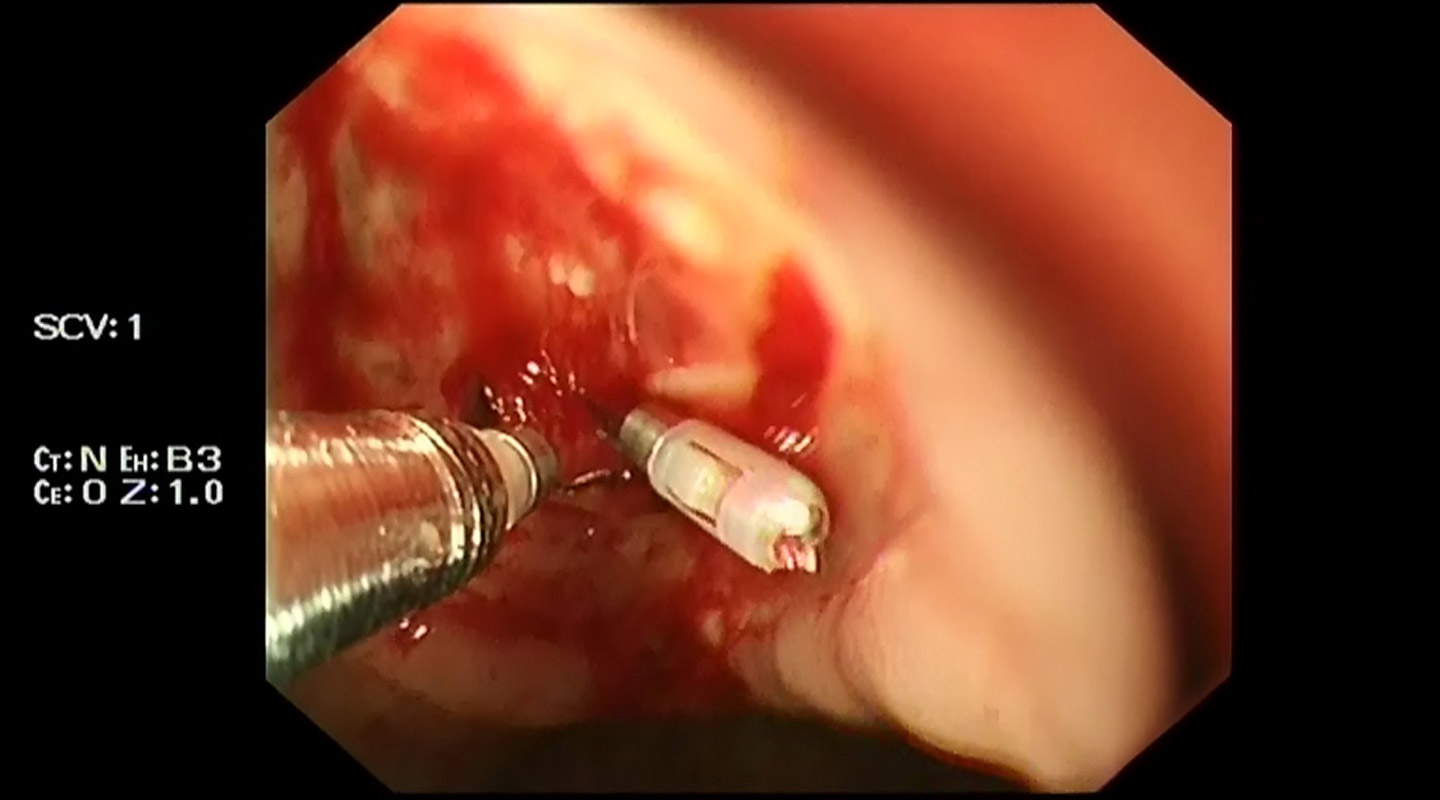
With a Croucher Senior Medical Research Fellowship, Professor Lau is leading an international research group to evaluate the significance of interventional radiology to endoscopic hemostasis treatment in patients with major bleeding. The study aims to determine whether preemptive angiographic embolization (AE) on patients with massive bleeding from peptic ulcer can reduce further bleeding and improve the treatment outcome.
A clinical trial involving 240 patients with bleeding gastro-duodenal ulcers requiring endoscopic hemostasis who fulfilled certain strictly defined criteria was carried out over a period of three years from 2010 to 2013. These patients were randomly divided into two groups of almost equal size, one of which was arranged to undergo AE treatment within 12 hours of endoscopy with high PPI dosage (the AE group) and the other with PPI alone (the non-AE group). The results showed that further bleeding in the AE group was around 4% compared with 11% in the non-AE group. The difference was more pronounced in cases with ulcers larger than 15 mm in size(a reduction by fivefold). There was zero 30-day mortality in the angiography group compared with 5% in the standard treatment group.
Professor Lau concluded that angiographic embolization should be offered to patients with larger ulcers after endoscopic treatment. The findings of this study are being put into a research paper, which may put down yet another marker in bleeding ulcer management.

There is no mystery in achieving success in research, as Professor Lau told us. To be curious and critical of the day-to-day clinical practice is the first big step. The design of the clinical research plan and a properly monitored process are critical. Although not all clinical trials have positive findings, carefully executed trials shall bring valuable evidence for further explorations and enhancements. Professor Lau believes that a good clinical research will eventually lead to positive changes and better the clinical practice. And, of course, it is most rewarding to see, at the end of the long process of many clinical trials, the patients benefit.
This article was originally published in No. 489/490, Newsletter in Dec 2016.